CDC, public health and regulatory officials in several states, and the U.S. Food and Drug Administration (FDA) are collecting different types of data to identify the food source of a multistate outbreak of Salmonella Telelkebir infections.
Epidemiologic data show that oysters may be contaminated with Salmonella and may be making people sick in this outbreak. CDC and FDA are working to determine the source of these oysters.
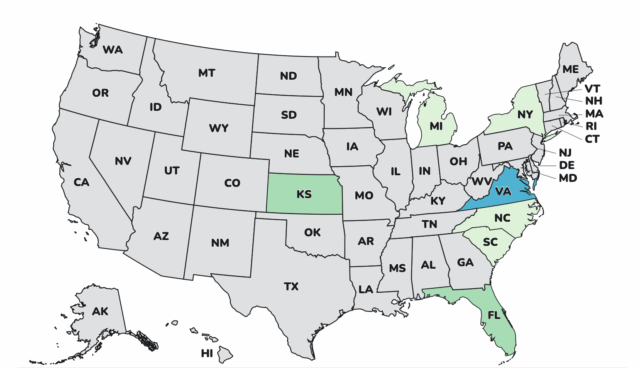
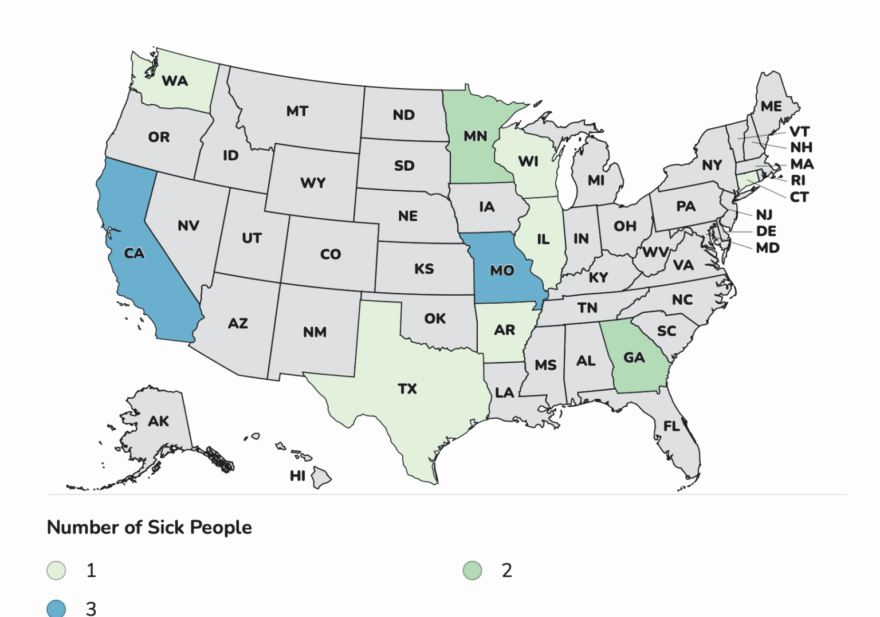
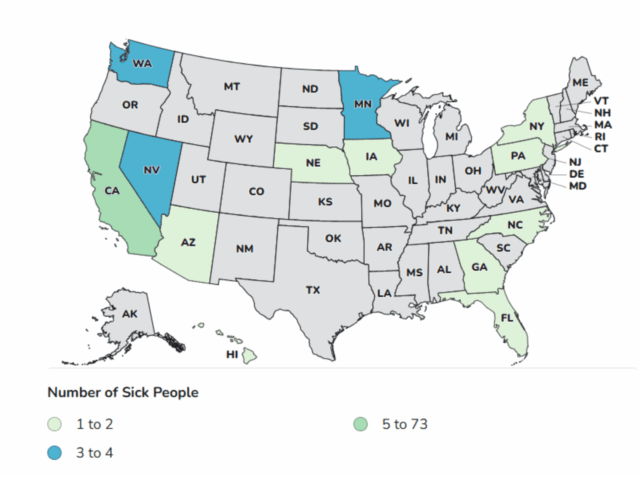
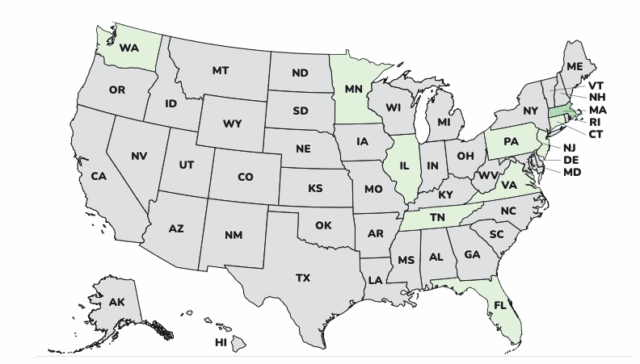
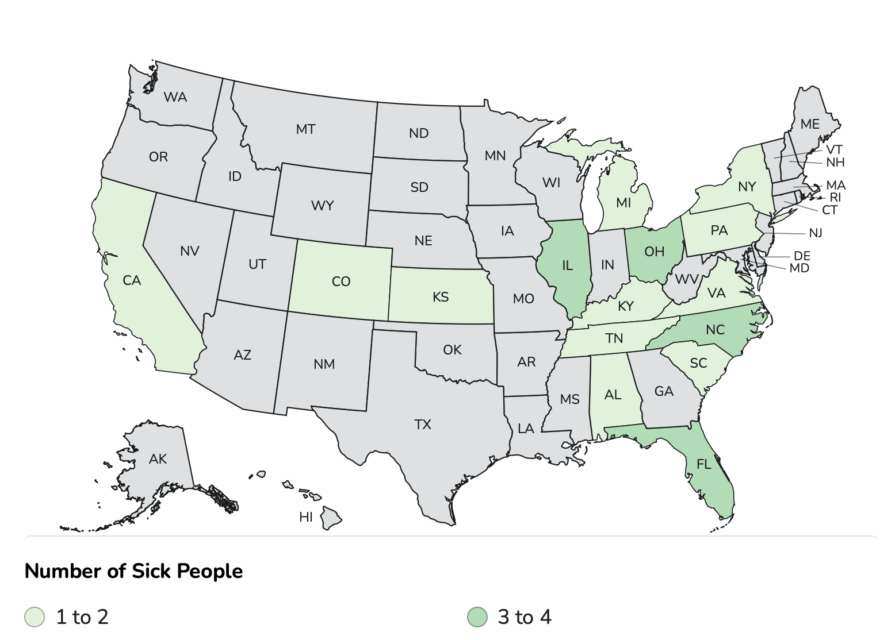
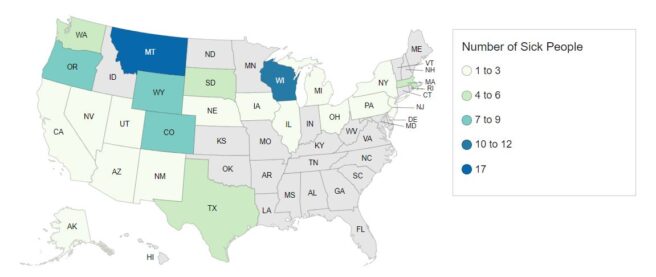
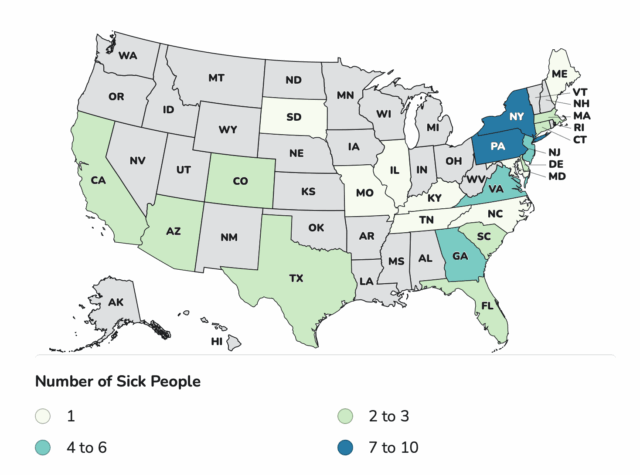
As of December 23, 2025, 64 people infected with the outbreak strain of Salmonella have been reported from 22 states: Illinois 1, Kentucky 1, Maine 1, Missouri 1, North Carolina 1, South Dakota 1, Tennessee 1, Maryland 1, Arizona 3, California 2, Colorado 3, Connecticut 2, Delaware 2, Florida 3, Massachusetts 3, South Carolina 3, Texas 2, Georgia 4, New Jersey 6, Virginia 6, New York 7, Pennsylvania 10.
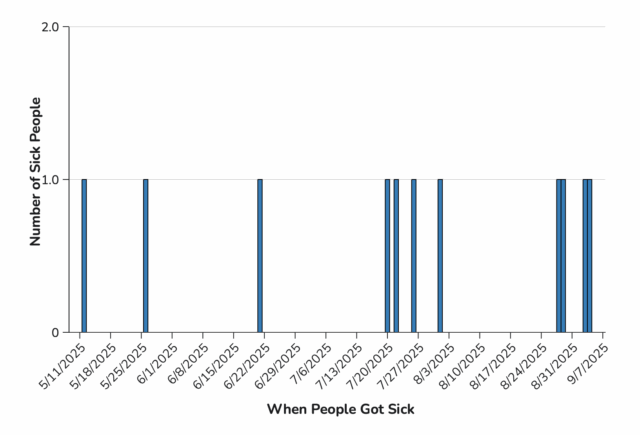
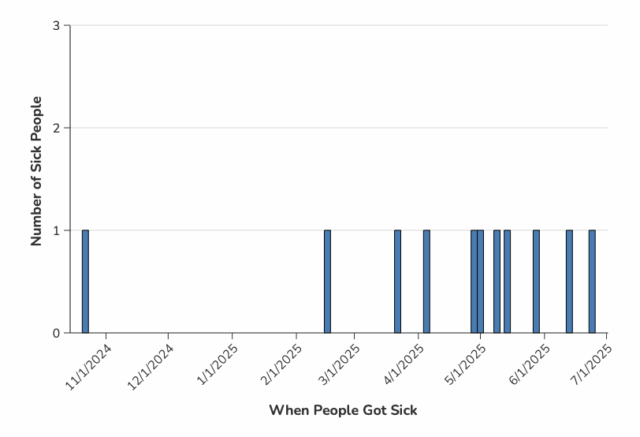
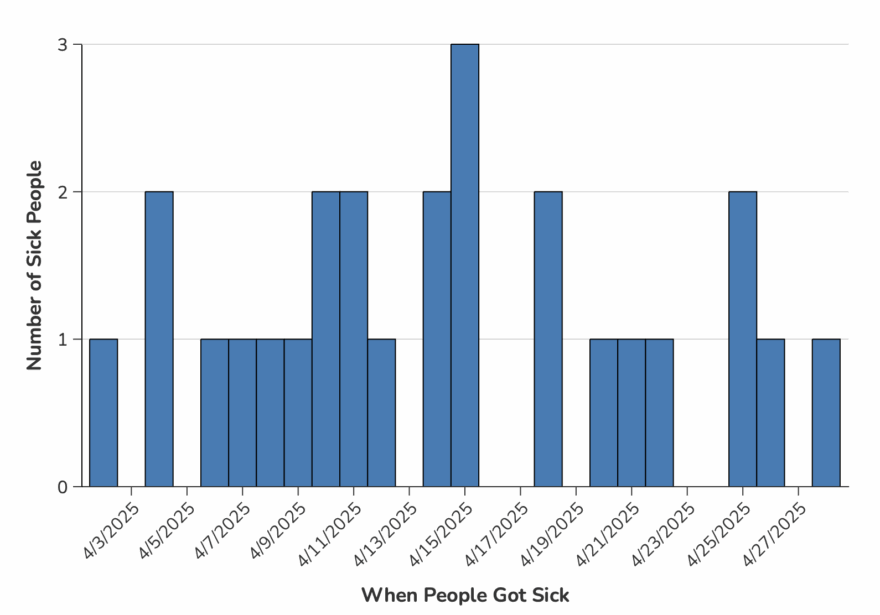
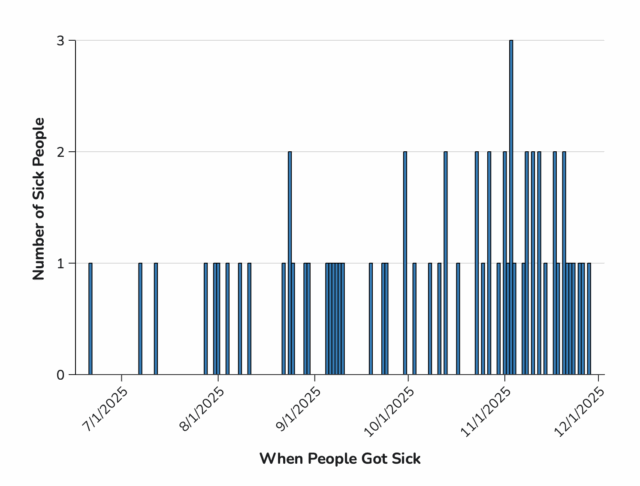
Illnesses started on dates ranging from June 21, 2025, to November 28, 2025. Of 44 people with information available, 20 have been hospitalized. No deaths have been reported.
The true number of sick people in this outbreak is likely much higher than the number reported, and the outbreak may not be limited to the states with known illnesses. This is because many people recover without medical care and are not tested for Salmonella. In addition, recent illnesses may not yet be reported as it usually takes 3 to 4 weeks to determine if a sick person is part of an outbreak.
Public health officials collect many different types of information from sick people, including their age, race, ethnicity, other demographics, and the foods they ate in the week before they got sick. This information provides clues to help investigators identify the source of the outbreak.
State and local public health officials are interviewing people about the foods they ate in the week before they got sick. Of the 27 people interviewed, 20 (74%) reported eating raw oysters. This percentage was significantly higher than the 1.6% of respondents who reported eating raw oysters in the FoodNet Population Survey—a survey that helps estimate how often people eat various foods linked to diarrheal illness. This difference suggests that people in this outbreak got sick from eating raw oysters.
Public health investigators are using the PulseNet system to identify illnesses that may be part of this outbreak. CDC PulseNet manages a national database of DNA fingerprints of bacteria that cause foodborne illnesses. DNA fingerprinting is performed on bacteria using a method called whole genome sequencing (WGS).
WGS showed that bacteria from sick people’s samples are closely related genetically. This suggests that people in this outbreak may have gotten sick from the same food.
Based on WGS analysis, bacteria from 59 people’s samples did not predict resistance to any antibiotics. More information is available at the National Antimicrobial Resistance Monitoring System (NARMS) site.
Raw oysters can be contaminated with germs at any time of year. Cook oysters before eating to reduce your risk of food poisoning.