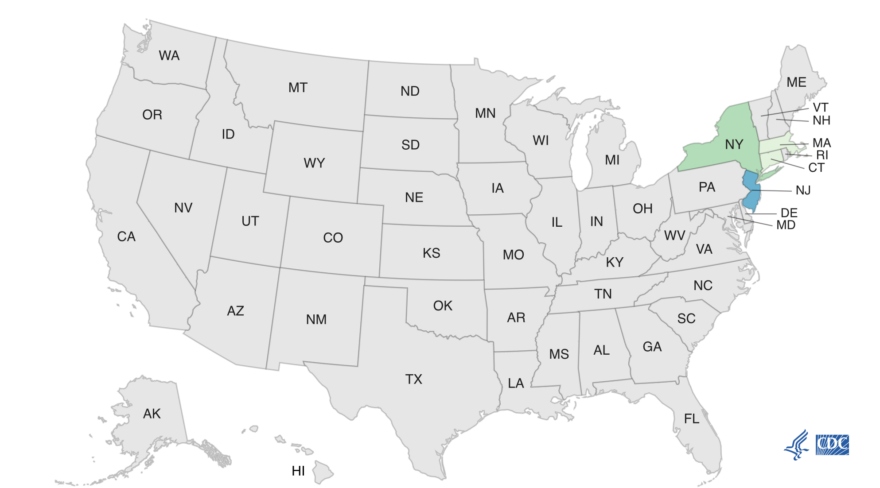
As of November 17, 43 people infected with the outbreak strain of Salmonella have been reported from 15 states. Illnesses started on dates ranging from October 17, 2023, to November 6, 2023. Of 30 people with information available, 17 have been hospitalized. No deaths have been reported.
Public health investigators are using the PulseNet system to identify